AIA Private Health insurance allows pre-approval for claims of any amount, no matter how small. Pre-approval provides you with peace of mind, and it means that your treatment costs can be paid directly to your health care providers. Please allow five working days for your pre-approval request to be processed. However, if your treatment is urgent then your request can be given priority.
File Online and Save Time
If you need to make a claim, or request pre-approval for a claim, you can do it online on the AIA website:
Make a Claim ›Pre-Approval Option
To obtain pre-approval for a procedure which is covered by your policy:
- Complete sections 1 to 4 of a Health Insurance Claim Form PDF.
- Ask your doctor to complete section 5 of the claim form, OR include a copy of a referral letter.
- The last page of the claim form does not need to be included until after the procedure.
- Send the claim form directly to AIA at the address below.
When seeking pre-approval, it is helpful (although not necessary) to provide an estimate of treatment costs. This can help to identify any issues with cover and to quantify any amount which you need to fund as a result of the excess you have chosen under your policy.
If you have any questions at all regarding pre-approval, or if you need help in completing a claim form, then phone a AIA team member on 0800 500 108.
When your treatment has been pre-approved, you will receive a confirmation letter which you can supply to your health care provider if required.
After you have had your treatment, complete the last page of the claim form, attach your providers’ invoices and forward to AIA at the address below.
Reimbursement Option
To obtain reimbursement for a covered event or procedure which you have already paid for:
- Complete sections 1 to 4 of a Health Insurance Claim Form PDF.
- Ask your doctor to complete section 5 of the claim form, OR include a copy of the referral letter.
- Complete the last page of the claim form and attach copies of the invoices you have paid.
- Send the claim form directly to AIA at the address below.
If you need help in completing the claim form, then phone AIA on 0800 500 108.
Claims Process
The entire claims process can be illustrated as follows:
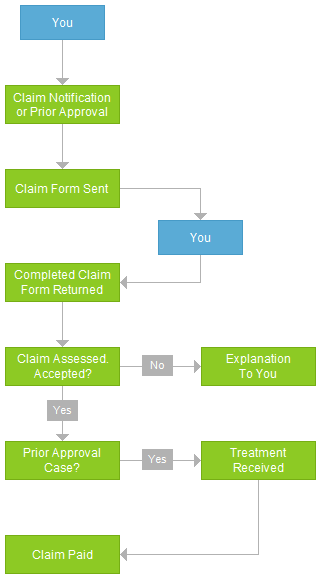
Claim Form
Health Insurance Claim Form PDF
Claim Submission
Whether for pre-approval or reimbursement, send your completed claim form and invoices to:
AIAPrivate Bag AIA
Victoria Street West
AUCKLAND 1142
